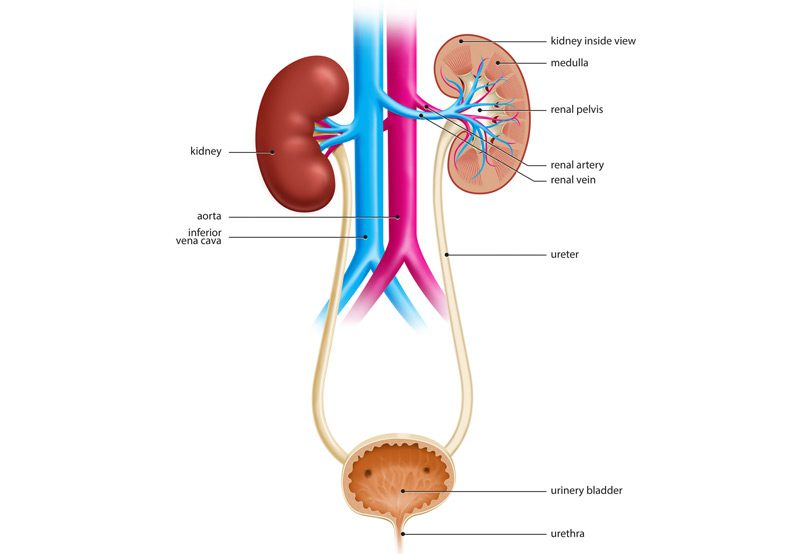
Male urinary incontinence treatment may involve medical therapy, bulking agent injections, male slings, Botox injections, and sacral neuromodulation.
Urinary incontinence (UI) affects about a quarter of all Americans. Patients with UI have difficulty controlling their bladder. Men with prostate-related symptoms and conditions are at an increased risk of developing bladder control issues.
While urinary incontinence is more common among older individuals, it’s not specifically limited to any one age group.
Medical Therapy
Male urinary incontinence treatment may involve medications such as anticholinergics and alpha blockers (for men) to help with symptoms.
Male Slings
The goal of a male sling procedure is to pull up and secure the bladder to narrow the urethra and minimize the risk of unexpected leakage from an overactive bladder. A “sling” is a piece of mesh that can be synthetic (manufactured) or created from a patient’s own tissue. In some cases, patients may have a sling made from donor tissue.
A sling is used to create a stretchable “hammock” just below the tube where urine travels out of the bladder. The sling is sometimes placed directly in the bladder neck, which is the spot where the bladder connects to the urethra.
Bulking Agent Injections
Bulking agent injections may be used to treat stress and urge incontinence. Stress incontinence is usually triggered by physical actions such as coughing or laughter. Patients experiencing urge incontinence are unable to hold urine until getting to a bathroom.
A urologist may treat male urinary incontinence with urethral bulking agents. Injections are usually recommended when patients haven’t experienced relief from exercises to strengthen pelvic floor and bladder muscles or medications that tighten bladder muscles or reduce contractions of the bladder.
OnabotulinumtoxinA (Botox) Injections
Botulinum toxin has been FDA-approved for bladder leaks caused by nerve damage. The procedure may also be used to treat patients experiencing issues with frequent urination and severe urge incontinence unrelated to an underlying problem with the urinary system.
Before receiving an injection of OnabotulinumtoxinA into the muscles of the bladder, patients will be asked to urinate to empty their bladder. A nurse will apply a local anesthetic gel to the area to minimize discomfort and reduce sensitivity. The injection will be administered using a lighted tube with a camera attached called a flexible cystoscope. The cystoscope will be inserted through the urethra into the bladder.
To make it easier to get the scope past the prostate gland, men may be asked to attempt to pass urine. Sterile water will be pumped into the bladder to expand the bladder’s lining and create a better view. The physician will make a series of injections during the procedure, which usually lasts about 15-20 minutes.
The injected toxin targets nerve endings to prevent muscular contractions. Patients may temporarily experience burning sensations during urination for a day or two after the injections. Overall, however, the risks of the procedure are minimal. Patients may need to look for signs of a urinary tract infection within the first few days after the injections.
Sacral Neuromodulation
During sacral neuromodulation, a small device is used to transmit electrical impulses to the sacral nerves, which are located by the tailbone. These nerves affect muscles in the bladder and parts of the pelvic area. Sacral nerves also play a role in controlling the sphincter and pelvic floor muscles, which play a role in bladder function.